Break Free from Chronic Pain and Mood Disorders with Ketamine Therapy
Discover a powerful solution for treatment-resistant conditions with our innovative ketamine therapy. Experience significant symptom relief and a path to healing with our expert team.
Fast-acting relief for depression, anxiety, PTSD, and chronic pain
Personalized care plans combining ketamine with holistic approaches
Proven efficacy with 70% of patients experiencing symptom reduction
“My boyfriend is a different person”
By my boyfriend’s second treatment, his agoraphobia, pain, limp, and depression were gone, and he continued to improve for the last four. Just a different person, the person I fell in love with. He was previously prescribed Suboxone but ketamine helped him come off of it.
-Alyssa K.
Ketamine debuted as a “buddy drug” during the Vietnam War, since it was so safe non-medical personnel could administer it on the battlefield for injuries. Multiple studies discovered ketamine’s antidepressant properties, and since that time, additional research has highlighted ketamine as an effect treatment for PTSD, OCD, bipolar depression, anxiety and panic disorders, fibromyalgia, Complex Regional Pain Syndrome, migraines, and other pain syndromes.
In most studies, about 70% of patients experience a significant reduction in symptoms – many during their first infusion. This is in comparison to a 16% efficacy rate after two medications have failed for those same syndromes. Ketamine is currently used by psychiatry and anesthesia providers to heal mood disorders, eliminate suicidal ideations, and reduce chronic pain.
Ketamine increases synaptogenesis and neuroplasticity, controls glutamate, and decreases inflammation.
Synaptogenesis is the formation of new connections between nerve cells in the nervous system. Neuroplasticity allows the brain to form and reorganize synaptic connections, especially in response to new information, new experiences, or following an injury. Glutamate is the primary fuel source for the central nervous system, but it worsens inflammation if not regulated properly, since it excites neurons. Inflammation is part of the body’s immune response to defend against invaders, but chronic inflammation and autoimmune disorders are quickly becoming an epidemic.

Negative Cycles
Our experiences strengthen or weaken synapses–the connections between neurons. Emotionally-charged memories form stronger connections, figuratively creating grooves in the brain. Both positive and negative impressions have the potential to strengthen their path in the brain. In the case of traumatic experiences, the brain may not be sure how to store the memory, and it’s reflected in physical symptoms as well as psychological issues. Pathways leading away from addiction or harmful coping mechanisms fade, and we get stuck in a rut with seemingly few options to deal with difficult situations. These cycles may be mental or physical and require neuroplasticity to create new patterns and beliefs.
When positive connections atrophy and negative patterns and behaviors are reinforced, people often despair in their depression.
The good news is that our brains are constantly re-shaping themselves, and, much like muscles, even the weakest positive connections can be strengthened with focused attention. We offer ketamine-assisted psychotherapy at our Akron ketamine clinic to enhance ketamine’s ability to reset brain connections and rise above past trauma and current hardships.
Harness the Power of Neauroplasticity with Ketamine

Ketamine for Mood Disorders
People affected with mood disorders frequently feel significantly better after receiving ketamine infusions. This is not because it tricks you into thinking you feel better. Ketamine helps repair the damage in the central nervous system caused by an incompetent NMDA receptor.
Ketamine, however, is not a cure for chronic disorders. It can be diagnostic, and we integrate care with our multi-disciplinary team and Ascend’s Friends in Northeast Ohio. Ketamine infusions address the root cause while starting the process of lessening symptoms.

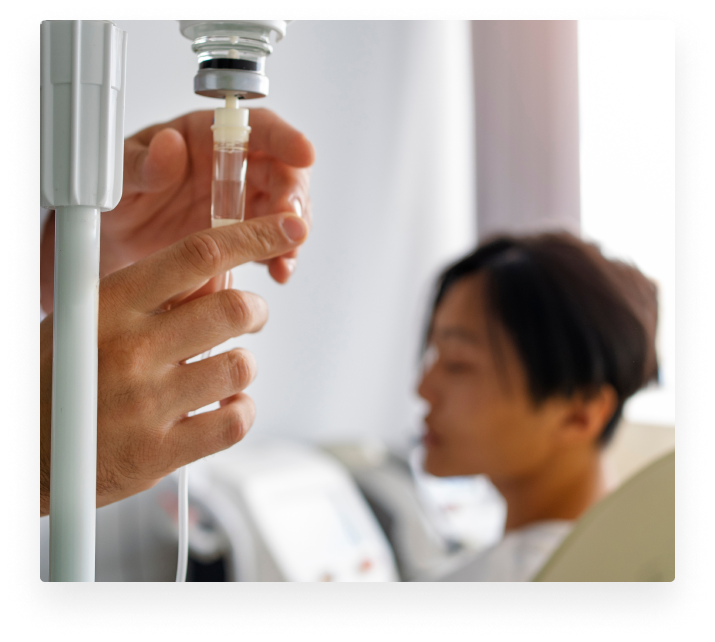
Ketamine for Pain Conditions
During your infusion, ketamine works on multiple receptors to help break cycles of chronic pain caused by nerve damage. Often our patients have elusive syndromes and only find us after multiple specialists gave conflicting diagnoses. Ketamine also has potent anti-inflammatory properties. We administer controlled doses of ketamine through an IV infusion lasting from one to four hours, and many patients find immediate relief from their chronic pain during their first infusion.
Re-Fuel Your Brain
Glutamate is the primary fuel source of the central nervous system. Mood disorders, in part, may be the result of our central nervous system (CNS) not having enough glutamate.
The N-Methyl-D-Aspartate (NMDA) receptor is like a dam for Glutamate. In mood disorders, the NMDA receptor may be dysfunctional and may remain open, allowing glutamate to flow freely in a very uncontrolled state. This decreases the amount of glutamate upstream from the NMDA receptor. When glutamate levels decrease to a critical level, the AMPA receptor stops functioning correctly. The AMPA receptor is responsible for neurogenesis (the formation of new nerve cells), neuroplasticity (the correct alignment of neurons), and controlling inflammation in the CNS. As the AMPA receptor frequently turns off, neurons begin shriveling up and dying off, and inflammatory processes become rampant.
Ketamine is a medication that works to slow down or stop the NMDA receptor from allowing the uncontrolled flow of glutamate through it. Ketamine selectively blocks the NMDA receptor which allows the CNS to fill back up with glutamate. Low dose intravenous Ketamine infusions only block the NMDA receptor for up to 72 hours. Therefore, multiple ketamine infusions are necessary to keep the NMDA receptor blocked until enough glutamate exists in the CNS to jump-start the AMPA receptor.
When the AMPA receptor is functional, it produces Brain-Derived Neurotrophic Factor (BDNF), which stimulates synaptogenesis, and increases neuroplasticity. Yoga, prayer, and exercise also stimulate BDNF, but at lower levels. In essence: it builds new neurons, helps neurons communicate effectively, and decreases inflammation. Once patients begin to feel better because of ketamine, we start incorporating nutrition and lifestyle changes; starting only with more subtle approaches if multiple medications have failed often just leads to discouragement.

Infusion Experience
We numb and clean the skin before placing an IV. The infusion runs on a precise medication pump, and patients describe their experiences as restful and peaceful. Many feel a greater acceptance for others and increased empathy and love, feeling more connected to God or the universe even after their first infusion. About 20% of our patients require maintenance infusions once a month or several times a year. This depends partly on the goals of treatment, whether weaning off pain and depression medication or trying to decrease suicide risk.


Mood disorders:
In our experience, 90% of clients experience significant reductions in symptoms.
65% experience sustained improvement in symptoms and do not come back for maintenance infusions.
For those with migraines and pain syndromes, additives to the ketamine extend the efficacy and can be used for breakthrough pain between infusions, along with specific supplements. In other cases, patients stay on their medications because now they work and additional infusions are not necessary.
Immediate Relief from Suicidal Ideations
Ketamine and Spravato provide fast relief in emergency suicidal situations. Suicidal intent with a plan is a medical emergency that needs to be treated in the emergency room. However, 14% of Americans have suicidal ideations which may need long-term supportive care.

Research and Studies
- Berman, R. M., Cappiello, A., Anand, A., Oren, D. A., Heninger, G. R., Charney, D. S., & Krystal, J. H. (2000). Antidepressant effects of ketamine in depressed patients. Biological Psychiatry, 47(4), 351-354. doi:10.1016/s0006-3223(99)00230-9. [PubMed]
- Murrough, J. W., Perez, A. M., Pillemer, S., Stern, J., Parides, M. K., Rot, M. A., . . . Iosifescu, D. V. (2013). Rapid and Longer-Term Antidepressant Effects of Repeated Ketamine Infusions in Treatment-Resistant Major Depression. Biological Psychiatry, 74(4), 250-256. doi:10.1016/j.biopsych.2012.06.022 [PubMed]
- Shiroma, P. R., Johns, B., Kuskowski, M., Wels, J., Thuras, P., Albott, C. S., & Lim, K. O. (2014). Augmentation of response and remission to serial intravenous subanesthetic ketamine in treatment resistant depression. Journal of Affective Disorders, 155, 123-129. doi:10.1016/j.jad.2013.10.036 [PubMed]
- Lapidus KA, Levitch CF, Perez AM, Brallier JW, Parides MK, Soleimani L, Feder A, Iosifescu DV, Charney DS, Murrough JW. 2014 A randomized controlled trial of intranasal ketamine in major depressive disorder. Biol Psychiatry. Dec 15;76(12):970-6. doi: 10.1016/j.biopsych.2014.03.026. Epub 2014 Apr 3 [PubMed]
- Michael Thase, MDK Ryan Connolly, MD, Unipolar depression in adults: Management of highly resistant (refractory) depression. [UpToDate][NIH Public Access]
- Mrazek DA, Hornberger JC, Altar CA, Degtiar I. A review of the clinical, economic, and societal burden of treatment-resistant depression: 1996-2013. 2014 Aug 1;65(8):977-87. doi: 10.1176/appi. ps.201300059. [PubMed]
FAQs
Low dose ketamine side-effects include nausea, anxiety, increased heart rate or blood pressure, and sedation, so we include medications with the infusion to decrease those risks.
We typically recommend 6-10 treatments over 3-4 weeks. Especially for an acute issue and when coupled with psychotherapy, this may be sufficient. Some patients require additional treatments on an as-needed basis, or we can combine infusions with Transcranial Magnetic Stimulation (TMS) for faster remission.
In some cases, intramuscular injections or nasal ketamine are administered at Ascend Health Center. SPRAVATO™, the brand name of esketamine, is a nasal medication derived from ketamine that was FDA-approved on March 5, 2019. Like TMS, we work with patients to get it covered by insurance if other treatments for depression or suicidality have failed.
It is approved, but please review the FDA’s website for more information. There are consensus statements from the American Psychiatric Association and the American Society of Anesthesiologists supporting utilizing IV ketamine for treatment resistant mood and neuropathic pain conditions. Ketamine was synthesized in 1963 and approved by the FDA in 1970. Medication trials prove a specific use of a drug to be safe and effective without significant side-effects. Once an older medication is approved, it is very rare for drug companies to spend the money required for additional research to put the medication “on label” for specific conditions–think of Benadryl uses beyond taking a small pink pill for itching.
SPRAVATO™ is a drug that was FDA-approved and covered by insurance for treatment-resistant depression and acute suicidality. It is a derivative of ketamine. During the research and drug development process, scientists isolated one side of the ketamine molecule to create a new version of the drug. Studies originally showed effectiveness in 50% of patients. We were the first clinic in our area to begin using SPRAVATO™ and the first in Ohio to administer SPRAVATO™ for the new indication of suicidal ideation. Our statistics show an efficacy of 80% at Ascend Health Center by integrating therapy and holistic approaches. Our anesthesia and psychiatry teams create individual plans with patients about the best treatment options. Patients are required to be monitored after using the nasal spray. The shortest appointments for established patients are about 30 minutes for small ketamine injections.
We provide the superior service of a self-pay model, but work with the patient and their insurance to determine the best path forward. Because time is money and deductibles may differ, an infusion while waiting for insurance to approve SPRAVATO™ or TMS is sometimes more affordable in the long run. As a ketamine clinic, we can also infuse or inject other medications, minerals, and vitamins depending on patient need. Our staff psychiatrist actively participates in patient care, and our nurse anesthetist administers all infusions as an extra measure of safety and expertise.
Response
Mood disorders:
- In our experience, 90% of clients experience significant reductions in symptoms.
- 65% experience sustained improvement in symptoms and do not come back for maintenance infusions.
- For those with migraines and pain syndromes, additives to the ketamine extend the efficacy and can be used for breakthrough pain between infusions, along with specific supplements. In other cases, patients stay on their medications because now they work and additional infusions are not necessary.